On this page:
- Disease it protects against
- Who should get the vaccine
- Why the vaccine is given in grade 6
- How well the vaccine works
- Safety
- Side effects
- How to manage side effects
- Who should not get the vaccine
- What if I am already sexually active?
- Other vaccines that protect against HPV
- HPV quick facts
- HPV vaccine videos
- HPV vaccine poster

Disease it protects against
- 7 types of HPV that cause about 90 percent of cervical cancers and several other cancers such as cancers of the vagina, vulva, anus, penis, mouth and throat.
- 2 types of HPV that cause about 90 percent of cases of genital warts.
Early protection works best!
The HPV vaccine is recommended sooner rather than later so that your child is protected long before they ever have contact with the virus.
Who should get the vaccine
- Grade 6 students
-
The HPV vaccine is offered for free to all students in grade 6. Most children in grade 6 need 2 doses of the vaccine to be protected. Children with a weakened immune system need 3 doses of the vaccine.
- Children and teens who missed the vaccine in grade 6
-
Those who miss getting the vaccine in grade 6 remain eligible for the free vaccine as long as:
- they get their first dose before they turn 19, and
- their last dose before they turn 26.
Those who miss getting the HPV vaccine in grade 6 can contact their immunization provider (i.e. local health unit, community health centre, health care provider, pharmacy) to make an appointment to get vaccinated.Children who get their first dose before their 15th birthday need 2 doses of the vaccine at least 6 months apart. People who get their first dose after their 15th birthday and those with a weakened immune system need 3 doses. - Some adults
-
The HPV vaccine is recommended and free for the following adults:
-
Males 19-26 years of age who are:
- Men who have sex with men (including those who are not yet sexually active and are questioning their sexual orientation).
- Street involved.
- Two-Spirit, transgender, and non-binary people 19-26 years of age.
The vaccine is recommended, but not free (unless mentioned above), for:- Women 19-45 years of age.
- Males 19-26 years of age.
- Males 27 years of age and older who have sex with men.
If you're not listed above and want to get the HPV vaccine, talk to your health care provider about your risk of getting an HPV infection and whether the vaccine would be right for you.
Those not eligible for the free vaccine can buy it at most pharmacies, travel clinics, and some sexual health clinics. Some health insurance plans cover the cost of the HPV vaccine. Check with your insurance provider to find out if your plan does.Adults need 3 doses of the vaccine. -
Males 19-26 years of age who are:
- People living with HIV
-
The vaccine is recommended and free for people 9-26 years of age who are living with HIV and have not received a complete series of the vaccine.
Why the vaccine is given in grade 6
- The vaccine works better at a younger age. Preteens make more antibodies after getting the vaccine than older teens or adults. This provides long-lasting protection against HPV.
- The vaccine works best when it is given before being exposed to the virus.
- Children in grade 6 only need 2 doses of the vaccine to be protected, while those 15 years and older (and those with a weakened immune system) need 3 doses.
Did you know?
More than 9 of every 10 cases of cervical cancer are caused by HPV. Almost all cervical cancer can be prevented by HPV vaccination.
How well the vaccine works
- Cancer-causing HPV infections.
- Cervical pre-cancers.
- Genital warts.
The HPV vaccine is very safe.
Hundreds of millions of doses of the HPV vaccine have been given safely worldwide. Over 15 years of safety monitoring show that the HPV vaccine is very safe and effective.
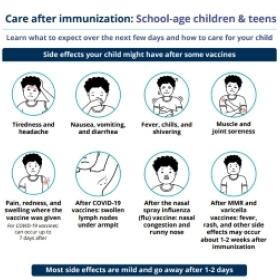
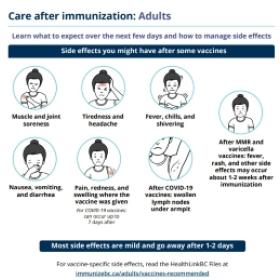
Side effects
- Pain, redness, or swelling in the arm where the vaccine was given.
- Fever.
- Dizziness or fainting.
- Nausea.
- Headache or feeling tired.
- Muscle or joint pain.
How to manage side effects
Who should not get the vaccine
- Speak with your health care provider if you or your child has had a life-threatening reaction to a previous dose of the HPV vaccine or any part of the vaccine, including yeast.
- People who are pregnant should not get the vaccine.
- There is no need to delay getting immunized because of a cold or other mild illness, but if you have concerns, speak with your health care provider.
What if I am already sexually active?
Cervical screening
It is important for people who have a cervix to follow current BC cervical screening guidelines because the HPV vaccine protects against most but not all types of HPV that cause cervical cancer.
Other vaccines that protect against HPV
HPV quick facts
- What is HPV?
-
HPV is the most common sexually transmitted infection (STI). About 3 out of 4 sexually active people who are unimmunized will get HPV at some time. Anyone who has any kind of oral, vaginal, or anal sexual contact can get HPV. Sexual intercourse is not necessary to get infected. The more sexual partners you have the higher the risk of being infected with HPV. Males who have sex with males are also at higher risk of HPV infection.
- How does HPV spread?
-
HPV spreads by skin-to-skin contact. This can be during oral, vaginal or anal sex or during any other sexual activity in which skin-to-skin contact takes place.
- What are the symptoms?
-
Most people infected with HPV do not show any signs or symptoms and can pass the virus on to others without even knowing it.Genital warts are a symptom of HPV infection. Genital warts are flat or cauliflower-like bumps that are usually painless, may be itchy, and sometimes bleed. They can be found in the groin, genitals, buttocks and inside the vagina or anus. They are rarely found in the mouth.
- What are the risks?
-
Most of the time, an HPV infection will clear on its own. For some people, HPV will not go away and cells infected with the virus can become precancerous or cancerous over time.Every year in B.C. approximately:
- 210 people will get cervical cancer and 55 will die from the disease.
- 6,000 people will develop high risk changes to the cervix which are precancerous.
- 135 people will get anal cancer and 20 will die from the disease.
- 5,500 people will develop genital warts.
HPV VACCINE VIDEOS
Cancer Prevention
Video courtesy of BC Cancer.
French | Mandarin | Punjabi | Cantonese
We Can Be the First
HPV: Our Family's Story
Audra and her aunt Laura are strong believers in the HPV vaccine, for a good reason: Gisel, Audra's mother and Laura's older sister, died from cervical cancer at only 38.